Amy Thoreson was the assistant director of the Scott County Health Department on March 12, 2020, when the COVID-19 virus arrived in the Quad-Cities. She and other public health officials met with school superintendents from across the county to discuss the possible courses of action.
For many people across the Quad-Cities, it was a time of unknowns and increasing anxiety.
Twenty-four hours before the meeting in Scott County, the University of Iowa, Iowa State University, and the University of Northern Iowa suspended in-person classes for two weeks. On March 13, Illinois Gov. JB Pritzker closed all schools until at least the end of March.
“It was a very uncertain time, and the information we were getting was changing very rapidly,” said Thoreson, who became director of the Scott County Health Department in 2021. “I remember the discussion was about if and when schools closed, one of the main questions was what would that look like for the greater community. The reality of the situation, for us at that time, was a lot of questions.”
People are also reading…
Another kind of reality hit Thoreson on her way home.
“I stopped into Target to pick up some things,” she recalled. “I remember standing in the toilet paper aisle and there wasn’t a single roll of toilet paper anywhere.
“I had been so focused on staying up with the public health side of things, I really hadn’t been paying attention to much else. I remember standing and thinking, ‘What is going on?’ It was eye-opening.”
Three days after that meeting, Iowa Gov. Kim Reynolds closed kindergarten through 12th-grade schools, saying they would be closed for at least a month. By March 21, Pritzker issued a stay-at-home order for the entire state of Illinois.
What followed was two years of uncertainties, mask mandates, controversies, vaccinations and booster shots, periods of widespread infection, widespread misinformation and the hope people could move on from the pandemic and get back to the way life was before anyone ever heard of COVID-19.
As we enter the third year of the pandemic, a number of public health and health care officials are still grappling with some questions raised by COVID-19.
What has been learned? What has changed?
That question, according to at least one local health official, may be premature.
“There have been a thousand possible impacts on public health already and it may be too early for even asking us this. The pandemic is not over and our ‘lessons learned’ are evolving and may materially change in coming months as it evolves,” Scott County Health Department Medical Director Dr. Louis Katz said.
Katz offered a broad perspective on where we’ve been and how that could influence where we go.
“The first thing one learns in ‘disaster preparedness and response 101’ is to have clearly defined and empowered command and control structures at every level. We did not have that in response to COVID from Day One, most damagingly at the federal level, even though it has been identified as critical for emergency response for decades,” Katz explained. “More than 2,800 state, counties, and large city health departments have operational public health authority, although often dominated by the state executive.
“We need to readjust federalism to allow ‘command and control’ to be more centralized, allowing broad and consistent evidence-based interventions and communications. This is a constitutional issue and will not be easy. A good start would be to return key public health appointments at the federal and state levels to the professional arena, as they used to be.”
Katz also stressed the need to “… rebuild the public health work force.”
While Katz focused on the broad aspects of what can be learned from the first two years of the pandemic, Barb Weber, chief operating officer, UnityPoint Health-Trinity, looked at a way the pandemic has changed procedure.
“During the pandemic, we saw a rapid rise in patients using telemedicine and expect that trend to continue,” Weber said. “It proved a critical tool during the height of the pandemic and continues to be a great resource for improving access to care especially in rural communities or to access specialty care. It has helped health professionals stay connected and monitor their patients safely.”
Doug Cropper, president and CEO, Genesis Health System pointed to changes Genesis made to meet the needs of its workforce during the pandemic.
“Probably one of the most interesting changes deals with the concept of ‘just-in-time’ inventory in supply-chain management. That concept goes out the window,” Cropper said. “The whole concept of global management of supplies and just-in-time inventory has to be rethought completely. In these days of global pandemics, or even global conflict if you look at Ukraine right now, can we truly have so many supplies that are critical for the United States produced outside of the country?
“Genesis decided early on, at the invitation of our buying group, Premier, to participate with 16 other health systems to invest in ownership of Prestige Ameritech in order to help ensure a steady flow of PPE supplies manufactured here in the United States.”
What is reality? Have communities fractured?
As the COVID-19 pandemic unfolded, sharp divisions — driven first by anti-lockdown sentiments and eventually issues like vaccine safety — appeared along political lines.
Rock Island County Health Department COO and Public Information Officer Janet Hill was one of the first local health official to speak out about how COVID-19 was being used as the political football.
“The amount of information — both true and false — that people are consuming about the pandemic has been staggering. From the beginning, public health has tried to be as consistent as possible, even when the situation was evolving quickly,” Hill said. “SARS-CoV-2 is a new virus, so scientists are learning about its characteristics in real-time. Sometimes, the information we passed along changed, which was confusing for many and allowed for seeds of distrust to be sown.
“Because of this avalanche of information, disinformation and misinformation, some people had trouble figuring out what to believe and what sources to trust. The politically-charged national media landscape and polarized social media feeds then allowed disinformation to be spread quickly, blunting proven prevention interventions, including masking, social and physical distancing, and, later, vaccines … . The pandemic never should have devolved into a political battle. Saving lives and caring for you, your family, and your community never should have been political.”
Katz was even more blunt. And he underlined a need for public health officials to find ways to better communicate with the public.
“We need to deal with the apparent inability for people to agree at a basic level about what is ‘true.’ Defining and confronting dangerous misinformation is a daunting task testing the appropriate balance between individual rights and public health — very difficult in the age of social media and the fragmentation of our communities that it both reflects and amplifies,” Katz said.
“We need to look very carefully at how, as public health officers, we convey and discuss the uncertainty that is the absolute and necessary nature of evolving scientific inquiry. This requires very clear, declarative statements about what we believe to be true that must especially include our ‘confidence intervals’ around the data that supports those judgments.”
Katz said public health had to help people understand how to critique evidence, and young people should leave schools with basic levels of critical and scientific literacy.
Much as sacrificed — but there is hope
As Thoreson recalled the start of the pandemic, she talked about some of things families sacrificed along the way. Hospitals and nursing homes closed visitation, leaving patients alone, or only allowed to look through a window at loved ones outside the facility. Medical workers changed their routines, with some living separated from family, to avoid bringing COVID home. Funeral homes started holding drive-thru visitations because larger gatherings could become COVID-spreader events and were off-limits. Schooling moved online, which proved helpful for some but difficult for many. Bus drivers in some districts continued their routes, delivering school lunches to students in need. Schools organized car parades to keep connected with students.
“The pandemic started to ramp up, and it was spring break time for a lot of families,” she said. “We had a family trip — including my dad — planned for Florida.
“Like a lot of families all over over the country, we canceled. As a public health official, I was starting to get a sense of just how dangerous that time was for people everywhere.
“And then the pandemic changes things bit by bit. My husband works in a hospital — so there was constant worry about what he could bring home. Our family changed — I was a public health employee during a pandemic. That came, in a lot of ways, before being a mom. I’m like a lot of parents out there — it’s like I’ve missed out on a lot of time with my family.”
Thoreson, however, holds on to hope.
“If you don’t have hope, there’s not a lot left for you,” she said. “We’ve weathered omicron. Things are better now, and maybe people will see that a tool like the vaccine can help things stay better.
“I have hope. I still believe we will get through this together.”
Covid-19 photos: Education in the Quad-Cities
032720-qc-nws-augie-039
Augustana College student Haley DeGreve works on her class work Friday at her Rock Island home.
032720-qc-nws-augie-037

Augustana College student Haley DeGreve works on her class work Friday, March. 27, at her Rock Island home.
032720-qc-nws-augie-048

Augustana College student Haley DeGreve works on her class work Friday, March. 27, at her Rock Island home.
032720-qc-nws-augie-036

Augustana College student Haley DeGreve works on her class work Friday, March. 27, at her Rock Island home.
032720-qc-nws-augie-041

Augustana College student Haley DeGreve works on her class work Friday, March. 27, at her Rock Island home.
032720-qc-nws-augie-044

Augustana College student Haley DeGreve works on her class work Friday, March. 27, at her Rock Island home.
032720-qc-nws-augie-043

Augustana College student Haley DeGreve works on her class work Friday, March. 27, at her Rock Island home.
032420-qc-nws-augie-059

Standing on a second floor balcony with his laptop, Augustana College senior, Tristan Odenkirk keeps close to the college campus as he stays at his student rental house with fellow students, Thursday, March. 26, in Rock Island.
032420-qc-nws-augie-053

Heading outdoors with his laptop, Augustana College senior Tristan Odenkirk keeps close to the college campus as he stays at his student rental house with fellow students, Thursday, March. 26, in Rock Island.
032420-qc-nws-augie-048

Cleaning dishes Augustana College senior Tristan Odenkirk keeps close to the college campus as he stays at his student rental house with fellow students, Thursday, March. 26, in Rock Island.
032420-qc-nws-augie-042

Working on his laptop computer Augustana College senior Tristan Odenkirk keeps close to the college campus as he stays at his student rental house with fellow students, Thursday, March. 26, in Rock Island.
032520-qc-nws-sherrardgrads-019

Shelley Zucker, with Jostens, waits to pass out caps and gowns Wednesday, March 25, 2020, at Sherrard High School. Students ordinarily would pick up their caps and gowns at school, but due to the COVID-19 virus, they were passed out individually while students and families waited in their cars.
032520-qc-nws-sherrardgrads-014

Elizabeth Steckel smiles after retrieving her cap and gown in March at Sherrard High School. Students ordinarily would pick up their caps and gowns at school, but due to the COVID-19 virus, they were passed out individually while students and families waited in their cars.
032520-qc-nws-sherrardgrads-015

Frank Zucker, with Jostens, hands Colton Bishop his cap and gown Wednesday, March 25, 2020, at Sherrard High School. Students ordinarily would pick up their caps and gowns at school, but due to the COVID-19 virus, they were passed out individually while students and families waited in their cars.
032520-qc-nws-sherrardgrads-018

Frank Zucker, with Jostens, hands Cody James his cap and gown Wednesday, March 25, 2020, at Sherrard High School.
032520-qc-nws-sherrardgrads-008

Katelin Hatlestad smiles as she waits to retrieve her cap and gown Wednesday, March 25, 2020, at Sherrard High School. Students ordinarily would pick up their caps and gowns at school, but due to the COVID-19 virus, they were passed out individually while students and families waited in their cars.
032520-qc-nws-sherrardgrads-004

Peyton Bradarich retrieves his cap and gown while sitting in his car Wednesday, March 25, 2020, at Sherrard High School. Students ordinarily would pick up their caps and gowns at school, but due to the COVID-19 virus, they were passed out individually while students and families waited in their cars.
032520-qc-nws-sherrardgrads-001

Frank Zucker, with Jostens, gives Lauren McMillin her cap and gown Wednesday, March 25, 2020, at Sherrard High School. Students ordinarily would pick up their caps and gowns at school, but due to the COVID-19 virus, they were passed out individually while students and families waited in their cars.
032520-qc-nws-sherrardgrads-002

Frank Zucker, with Jostens, hands Sarah Sorrell her cap and gown Wednesday, March 25, 2020, at Sherrard High School. Students ordinarily would pick up their caps and gowns at school, but due to the COVID-19 virus, they were passed out individually while students and families waited in their cars.
032520-qc-nws-sherrardgrads-003

Shelley Zucker, with Jostens, hands Emma Hofmann her cap and gown Wednesday, March 25, 2020, at Sherrard High School. Students ordinarily would pick up their caps and gowns at school, but due to the COVID-19 virus, they were passed out individually while students and families waited in their cars.
032520-qc-nws-sherrardgrads-016

Frank Zucker, with Jostens, hands Carley Whitsell her cap and gown Wednesday, March 25, 2020, at Sherrard High School. Students ordinarily would pick up their caps and gowns at school, but due to the COVID-19 virus, they were passed out individually while students and families waited in their cars.
032520-qc-nws-sherrardgrads-011

Joshua Eberts retrieves his cap and gown Wednesday, March 25, 2020, at Sherrard High School. Students ordinarily would pick up their caps and gowns at school, but due to the COVID-19 virus, they were passed out individually while students and families waited in their cars.
032520-qc-nws-sherrardgrads-009

Katelin Hatlestad smiles after retrieving her cap and gown Wednesday, March 25, 2020, at Sherrard High School. Students ordinarily would pick up their caps and gowns at school, but due to the COVID-19 virus, they were passed out individually while students and families waited in their cars.
032520-qc-nws-sherrardgrads-012

Frank Zucker, with Jostens, hands Kacey Plambeck his cap and gown Wednesday, March 25, 2020, at Sherrard High School. Students ordinarily would pick up their caps and gowns at school, but due to the COVID-19 virus, they were passed out individually while students and families waited in their cars.
032520-qc-nws-sherrardgrads-017

Frank Zucker, with Jostens, hands Tyler Scott his cap and gown Wednesday, March 25, 2020, at Sherrard High School.
032520-qc-nws-sherrardgrads-013

Taylor Williams smiles after retrieving her cap and gown Wednesday, March 25, 2020, at Sherrard High School. Students ordinarily would pick up their caps and gowns at school, but due to the COVID-19 virus, they were passed out individually while students and families waited in their cars.
032520-qc-nws-sherrardgrads-005

Frank Zucker, with Jostens, hands Jacob Young his cap and gown Wednesday, March 25, 2020, at Sherrard High School. Students ordinarily would pick up their caps and gowns at school, but due to the COVID-19 virus, they were passed out individually while students and families waited in their cars.
032520-qc-nws-sherrardgrads-006

Kyli Newton holds the remaining balance for her cap and gown before retrieving it Wednesday, March 25, 2020, at Sherrard High School. Students ordinarily would pick up their caps and gowns at school, but due to the COVID-19 virus, they were passed out individually while students and families waited in their cars.
032520-qc-nws-sherrardgrads-007

Katelin Hatlestad smiles as she waits to retrieve her cap and gown Wednesday, March 25, 2020, at Sherrard High School. Students ordinarily would pick up their caps and gowns at school, but due to the COVID-19 virus, they were passed out individually while students and families waited in their cars.
032320-qc-nws-lunch-008

Siblings Hannah, 15, Kayla, 15, and Jordan Rice, walk up to pick up meals Monday, March 23, 2020, at Rock Island High School. The Rock Island-Milan School District offered a pick up meal service for all students. The meal kit included 3-day meal packages with breakfast and lunch.
032320-qc-nws-lunch-001

Craig Sharp hands Rock Island student Jordan Rice a box of meals Monday, March 23, 2020, at Rock Island High School. The Rock Island-Milan School District offered a pick up meal service for all students. The meal kit included 3-day meal packages with breakfast and lunch.
032320-qc-nws-lunch-016

Meaghan Jackson gives a meal kit to a parent Monday, March 23, 2020, at Rock Island High School. The Rock Island-Milan School District offered a pick up meal service for all students. The meal kit included 3-day meal packages with breakfast and lunch.
032320-qc-nws-lunch-013

Lakisha Randle picks up a meal kit Monday, March 23, 2020, at Rock Island High School. The Rock Island-Milan School District offered a pick up meal service for all students. The meal kit included 3-day meal packages with breakfast and lunch.
032320-qc-nws-lunch-017

A person takes a schoolwork packet Monday, March 23, 2020, at Rock Island High School. The Rock Island-Milan School District offered a pick up meal service for all students. The meal kit included 3-day meal packages with breakfast and lunch.
032320-qc-nws-lunch-011

Siblings Kayla, 15, Jordan, Hannah, 15, and Olivia Rice, 13, walk back home with their meal kits Monday, March 23, 2020, at Rock Island High School. The Rock Island-Milan School District offered a pick up meal service for all students. The meal kit included 3-day meal packages with breakfast and lunch.
032320-qc-nws-lunch-010

Rock Island student Jordan Rice picks up a box of meals Monday, March 23, 2020, at Rock Island High School. The Rock Island-Milan School District offered a pick up meal service for all students. The meal kit included 3-day meal packages with breakfast and lunch.
032320-qc-nws-lunch-004

Laura Irish assists parents as they come to pick up meals Monday, March 23, 2020, at Rock Island Academy. The Rock Island-Milan School District offered a pick up meal service for all students. The meal kit included 3-day meal packages with breakfast and lunch.
032320-qc-nws-lunch-003

Laura Irish assists parents as they come to pick up meals Monday, March 23, 2020, at Rock Island Academy. The Rock Island-Milan School District offered a pick up meal service for all students. The meal kit included 3-day meal packages with breakfast and lunch.
032320-qc-nws-lunch-005

A carton of milk is laid out for students and parents to pick up Monday, March 23, 2020, at Rock Island Academy. The Rock Island-Milan School District offered a pick up meal service for all students. The meal kit included 3-day meal packages with breakfast and lunch.
032320-qc-nws-lunch-019

Laura Irish grabs cartons of milk for parents as they come to pick up meals Monday, March 23, 2020, at Rock Island Academy. The Rock Island-Milan School District offered a pick up meal service for all students. The meal kit included 3-day meal packages with breakfast and lunch.
032320-qc-nws-lunch-002

People work to bag up the meal kits Monday, March 23, 2020, at Rock Island Academy. The Rock Island-Milan School District offered a pick up meal service for all students. The meal kit included 3-day meal packages with breakfast and lunch.
032320-qc-nws-lunch-012

People await parents and students to give meal kits and schoolwork packets to Monday, March 23, 2020, at Rock Island High School. The Rock Island-Milan School District offered a pick up meal service for all students. The meal kit included 3-day meal packages with breakfast and lunch.
032320-qc-nws-lunch-009

Rock Island student Jordan Rice walks up to pick up a meal kit Monday, March 23, 2020, at Rock Island High School. The Rock Island-Milan School District offered a pick up meal service for all students. The meal kit included 3-day meal packages with breakfast and lunch.
032320-qc-nws-lunch-015

Craig Sharp helps Lakisha Randle with loading cartons of milk into her car Monday, March 23, 2020, at Rock Island High School. The Rock Island-Milan School District offered a pick up meal service for all students. The meal kit included 3-day meal packages with breakfast and lunch.
032320-qc-nws-lunch-018

Items that would be included in a meal kit are laid out Monday, March 23, 2020, at Rock Island Academy. The Rock Island-Milan School District offered a pick up meal service for all students. The meal kit included 3-day meal packages with breakfast and lunch.
032320-qc-nws-lunch-007

Meaghan Jackson and Michelle Lillis box up meals for students and parents to pick up Monday, March 23, 2020, at Rock Island High School. The Rock Island-Milan School District offered a pick up meal service for all students. The meal kit included 3-day meal packages with breakfast and lunch.
032320-qc-nws-lunch-006

Michelle Lillis, athletic director, laughs as she boxes up meals for parents and students to pick up Monday, March 23, 2020, at Rock Island High School. The Rock Island-Milan School District offered a pick up meal service for all students. The meal kit included 3-day meal packages with breakfast and lunch.
032320-qc-nws-lunch-014

Lakisha Randle picks up a meal kit Monday, March 23, 2020, at Rock Island High School. The Rock Island-Milan School District offered a pick up meal service for all students. The meal kit included 3-day meal packages with breakfast and lunch.
032420-qc-nws-augie-07.JPG

Augustana senior Christian Elliott sits in the window of his parents home in Blue Grass, Iowa March 22, 2020.
032420-qc-nws-augie-05.JPG

Augustana senior Christian Elliott sits in the window of his room at his parents home in Blue Grass, Iowa March 22, 2020.
032420-qc-nws-augie-06.JPG

Augustana senior Christian Elliott sits in the window of his room at his parents home in Blue Grass, Iowa.
032420-qc-nws-augie-04.JPG

Justin Verlinden an Augustana College senior looks through the window of his home in Rock Island, March 21, 2020.
032420-qc-nws-augie-02.JPG

Justin Verlinden an Augustana College senior looks through the window of his home in Rock Island, March 21, 2020.
032420-qc-nws-augie-01.JPG

Justin Verlinden an Augustana College senior looks through the window of his home in Rock Island, March 21, 2020.
032420-qc-nws-augie-03.JPG

Justin Verlinden an Augustana College senior looks through the window of his home in Rock Island, March 21, 2020.
031620-qct-PepsiCo-04.JPG

Samridha Rana, 21, of Nepal plays basketball with his friend Ashin Adhikari, 19, at the PepsiCo Recreation Center at Augustana Monday, March 16, 2020.
031620-qct-PepsiCo-05.JPG

International students play video games at the PepsiCo Recreation Center at Augustana Monday, March 16, 2020.
031620-qct-PepsiCo-01.JPG
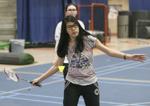
Trang Hoang 19, of Vietnam plays badminton at the PepsiCo Recreation Center at Augustana Monday, March 16, 2020.
031620-qct-PepsiCo-03.JPG

Nguyen Truong 21, of Vietnam plays badminton at the PepsiCo Recreation Center at Augustana Monday, March 16, 2020.
031620-qct-PepsiCo-06.JPG

Samridha Rana, 21, of Nepal plays basketball at the PepsiCo Recreation Center at Augustana Monday, March 16, 2020.
031620-qct-PepsiCo-02.JPG

Ashin Adhikari, 19, of Nepal plays basketball with his friend Samridha Rana, 21, at the PepsiCo Recreation Center at Augustana Monday, March 16, 2020.








